New Patients: (561) 609-6491
Existing Patients: (561) 395-0550
7280 W Palmetto Park Rd
Suite 206N
Boca Raton, FL 33433

At the office of Marisol Ruiz, DMD, our patients' care and well-being are our top priorities. Every member of our skilled and experienced team strives to ensure patient comfort and a stress-free dental experience. Our dedication to the consistent provision of compassionate and personalized attention along with gentle, precise care has earned our office the respect and trust of our patients.
While we do everything we can to preserve the integrity of your natural smile, it's sometimes necessary to extract a tooth to protect your oral health and overall well-being.
A "baby" or deciduous tooth that is over retained (reluctant to fall out), severely decayed, or damaged
In most cases, a baby tooth will fall out as scheduled as the underlying permanent one begins to erupt into place. However, occasionally a baby tooth continues to remain firmly attached to the bone. Either the roots of the baby tooth have failed to resorb and shrink as intended, or the baby tooth has become anklylosed and fused to the supporting bone. The problem is that over-retained baby teeth can disrupt the development and alignment of your child's smile. As we monitor your child's smile as they grow, we'll advise you if and when an extraction of a baby tooth is required to facilitate the eruption of its underlying permanent successor.
A permanent tooth that has extensive decay and is deemed non-restorable
Beginning as a simple pinpoint defect on the outermost enamel layer of your tooth, untreated dental decay will continue to compromise healthy tooth structure as it works its way to the inner layers of the tooth. Without proper care, a cavity can lead to significant damage to tooth structure, irreversible damage to the nerve of the tooth, a dental infection, and serious consequences to your oral health and overall well-being. When the tooth has sustained far too much structural damage and cannot be restored, a dental extraction may be required.
A permanent tooth that has been severely fractured or cracked and can not be restored
There are many different types of chips, cracks, and fractures that can affect your teeth. The extent of the damage that it causes will determine if there is enough intact tooth structure to save the tooth and the type of treatment required. In cases where too much tooth structure or the root of a tooth has also been compromised, an extraction may be necessary.
Advanced gum disease that has significantly compromised the tooth's supporting tissues
The most common cause of tooth loss in adults is gum disease. When left untreated, periodontal disease, which affects the hard and soft tissues supporting your teeth, can lead to gingival pocket formation, gum recession, and diminishing alveolar bone. As advanced and untreated gum disease progresses, the teeth ultimately loosen, fall out, or require extractions.
Poorly positioned, impacted, or decayed wisdom teeth
Wisdom teeth, which are also known as the third molars, are the last permanent teeth to develop in the oral cavity and the final ones to come into place. However, as is often the case, many wisdom teeth do not have sufficient room to erupt, are not developing correctly, develop extensive decay, or cause issues for the adjacent teeth and the surrounding tissues. Although the extraction of wisdom teeth sometimes gets recommended for an older patient, the early removal of troublesome or potentially problematic third molars in young adults is more often the case.
Overcrowded Teeth
A tooth size to jaw size discrepancy often results in a crowded and misaligned smile. More simply put, the upper and lower jaws are not large enough to accommodate all the permanent teeth. As part of an orthodontic treatment plan to optimally align teeth and establish an attractive, healthy, and functional bite, the extraction of select permanent teeth may be required.
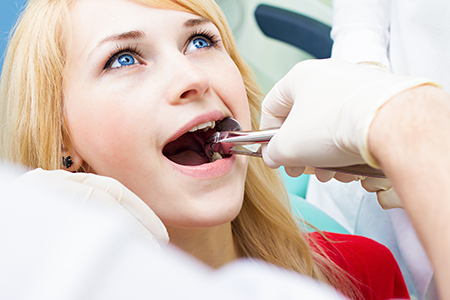
Whatever the reasons for a dental extraction may be, you can rest assured that your care is in the best of hands at our office. As the first step in care, our dentist will review your medical and dental histories and discuss any special considerations in care.
It's essential to inform our office of any existing medical conditions or medications you are currently taking. In some situations, extra precautions, including premedication with antibiotics, a change in medication, and a medical clearance may be required. Follow all our pre-surgical directives and let us know if you are sick or have developed other symptoms on the day of surgery.
Our goal is to reduce any anxiety and help ensure patient comfort whenever a tooth extraction is necessary. In advance of the procedure, we'll discuss any medical considerations or precautions and go over our pre-surgical instructions. We'll also discuss post-surgical recommendations, including whether replacing the extracted tooth or teeth is needed and the best options in care.
To thoroughly assess the tooth and the type of extraction required, we perform a comprehensive examination and take digital radiographs as indicated. Extractions are typically categorized as either "simple" or "surgical extractions."
When the tooth is clearly visible in the mouth and the root anatomy is not extensively hooked, fused to the surrounding bone, or otherwise unusual, it usually falls into the category of a simple extraction. Once the tooth and the surrounding tissues get sufficiently numbed with a local anesthetic, our dentist will loosen any attached periodontal tissues and apply forceps to remove the tooth. As with all dental procedures, we do all we can to help ensure your comfort and relaxation throughout every step in care. For patients who are anxious about dental work or certain procedures, we can discuss additional options in dental sedation.
For teeth that are severely broken down, anklylosed, or impacted, a surgical extraction is often indicated. We may refer you to an oral and maxillofacial surgeon to perform this procedure. During a surgical extraction, a small incision in the soft tissues and localized, precise removal of overlying bone provides greater access to remove the tooth. As with all tooth extractions, patients are given a local anesthetic to completely numb the involved tooth and the surrounding tissues. Once again, additional options in dental sedation, pre-surgical considerations, and directives are thoroughly discussed and explained.

As skilled and experienced providers of care, we recognize that every case is different and provide treatment that addresses the unique requirements of each patient. Depending on a patient's specific needs, we provide post-operative instructions, including special instructions, limitations on activities, medications, and follow-up care that support optimal recovery and healing. In some cases, post-op care may also include the involvement of a patient's physician. In general, and unless modified otherwise by our office, the following post-operative guidelines apply to simple extractions.
Maintaining gauze pressure
Following your extraction, some gauze to bite down on will be placed over the extraction site. By biting down and maintaining pressure on the gauze as instructed, any active bleeding should stop. You may change the gauze pad after the first hour. Continue to bite down for another 45 minutes if heavy oozing continues. While it's normal for a little oozing to continue for 24 hours, contact our office if you are still experiencing profuse oozing or bleeding.
Until the local anesthesia wears off
Until the local anesthetic has completely worn off, it's essential to protect yourself from unintentionally biting or injuring your lips, cheeks, gums, or tongue.
Take medications as prescribed
Antibiotics:
If you have been given a prescription for antibiotics, be sure to take the correct dosage and full course of medication as prescribed.
Pain management:
It's helpful to take a pain reliever before the local anesthetic completely wears off. Over-the-counter (non-aspirin) pain medication may be taken to relieve discomfort. Any prescription pain medication should only be taken as directed.
To facilitate healing
Do not rinse your mouth, spit, drink through a straw, or suck on candies. It's essential to allow the extraction site to clot and not dislodge the new clot once it has formed.
Applying ice
An ice-pack held in place in the facial area overlying the extraction site helps to control swelling. Apply the ice for 10-minute intervals during the first day following your procedure.
Avoid smoking
Smoking not only prevents clot formation, but it also interferes with healing. Avoid smoking and tobacco products for the first week.
Watch what you eat and drink
Stay away from hot or spicy foods and drinks for the first day or two. Also, refrain from drinking any carbonated or alcoholic beverages. Stick with a diet of soft foods and liquids for the first couple of days following surgery. Drink plenty of fluids.
Oral hygiene
Brush gently; it's essential to take great care not to disturb or irritate the extraction site for a few days. A very mild lukewarm saltwater solution can be used to freshen your mouth. Remember not to rinse or spit that first day or two. Simply let any liquids gently fall from your mouth into the sink.
An appointment for a follow-up visit
If sutures (stitches) were placed, or if a complex extraction, an infection, or other issues requires a visit to monitor your healing and progress, you will be given an appointment for follow-up care. It's essential that you keep this appointment as provided.
If you experience continued bleeding, ongoing pain, more swelling, have a bad taste in your mouth, or other unusual symptoms, contact our office.

You deserve quality care that's personalized to meet your individual needs, and at the office of Marisol Ruiz, DMD, you can rest assured your smile is in the best of hands. We deliver precise and gentle care, keeping you informed and relaxed throughout your procedure. If your tooth needs to be replaced, we'll discuss your best options, including dentures, fixed bridges, and dental implants. As the most advanced method of tooth replacement available, dental implants come the closest to replicating the look, feel, and function of a natural smile.